Breathing Obstruction
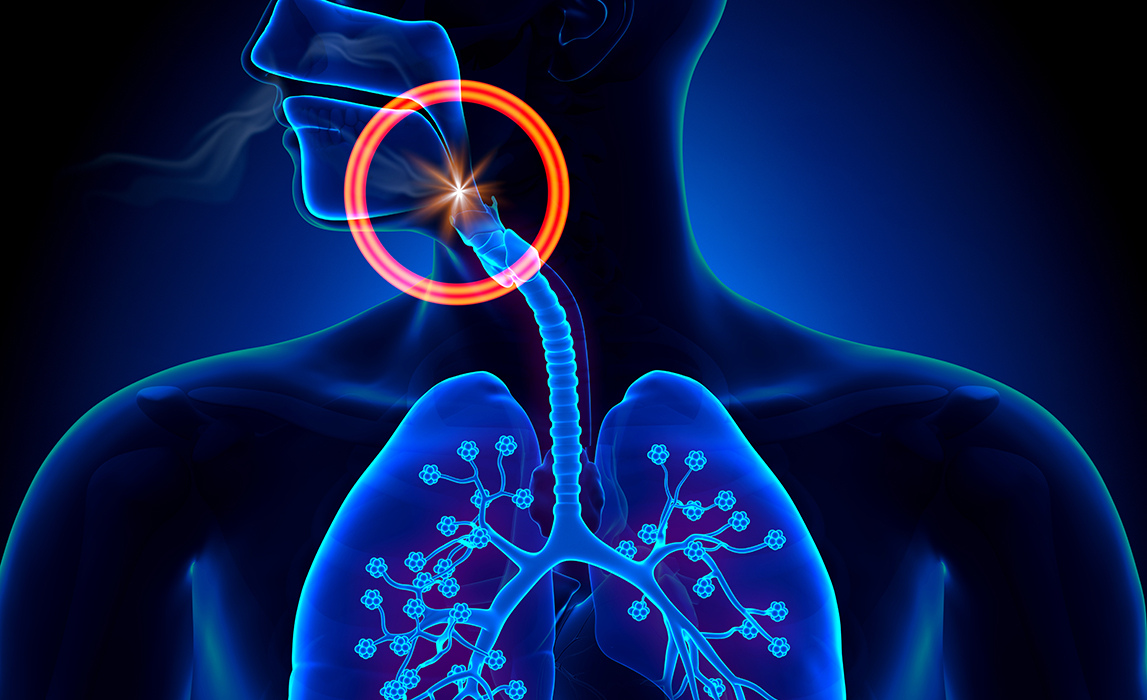
When an object fully or partially blocks the epiglottis (the flap at the back of your tongue that closes your throat when you swallow), breathing is stalled and air cannot inflate the lungs. Oxygen cannot be delivered to critical systems, resulting in rapid failure of all the body’s systems.
If you witness someone suffering from choking, it is important to react immediately and clear the airway. Blockage could be the result of large chunks of partially chewed food; alcohol consumption (which relaxes the epiglottis); swallowed dentures; laughing/talking while eating or eating too fast; or (especially with kids) objects in the mouth.
In the case of a partial obstruction, encourage coughing. You will hear a high-pitched wheezing sound known as “stridor” that results from turbulent airflow in the larynx (your voice box). Do not interfere with a victim’s coughing. If the coughing persists or the victim’s speech is slurring, call EMR *9999.
With an almost full or complete blockage, the victim’s color will change to blue. You should intervene with urgency. The universal sign of a victim who cannot breathe at all is clutching at the throat.
Observe the following protocol:
- Check the scene.
- Ask the person, “are you choking, can you cough?”
- Ask someone to call emergency response for help (*9999 in Ho Chi Minh City).
- Lean victim forward (in case of a child, over the knee).
- Administer five sharp blows to the back.
- Stand behind victim (in case of a child, kneel) with arms around the stomach.
- Perform five abdominal thrusts (the Heimlich maneuver) or chest thrusts for pregnant women.
- Alternate back blows and abdominal thrusts until the victim ejects the blockage.
- Check for loss of consciousness after every blow/thrust.
- If the victim loses consciousness, lie him/her down and follow basic life saving guidelines as for cardiac arrest: For adults, administer one ventilation every five–six seconds over two minutes.
For infants less than one year old, DO NOT USE HEIMLICH. Do CPR-style finger chest thrusts. For back blows, hold the child upside down and support under throat, strike 60% down the back. Rescue breaths—puff once with cheek air (not lung air) every three–four seconds.
 We use cookies on this website to enhance your user experience
We use cookies on this website to enhance your user experience